📅 Published on: May 20, 2024 | 🔄 Updated on: March 28, 2026 | By: Global Stem Cell Care India
Key Takeaways
- 01:Supporting Retinal Cell Repair and Regeneration: Retinal detachment can cause serious damage to delicate retinal cells. Stem cell treatment is focused on restoring the retina by stimulating the regrowth of dysfunctional photoreceptor cells. When the cells are transplanted, they become integrated with the layers of the retina, which enables the restoration of the pathway through which signals travel from the eye to the brain. The earlier it is done, the better, and progress can be monitored to make changes in the treatment if desired.
- 02:Preventing Further Retinal Degeneration: Stem cells not only repair damage but also protect existing retinal cells. They also reduce inflammation in areas with damage and slow down any progression that could occur. Early treatment increases the chances of retaining visual functions. The doctor closely monitors retinal integrity to identify any abnormalities early enough. Often, combining different therapies, such as helper drugs and vision therapy, could enhance outcomes.
- 03:Improving Visual Function and Daily Life: The retinal separation might have a significant impact on visual acuity and routine tasks. The vision repair therapy utilizing stem cells has the potential to bring partial vision to the affected areas, which improves light sensitivity, perception of depth, or color vision. Small amounts of vision advancements could bring immense benefits to routine life and autonomy. The therapy aims at functional vision and advancements rather than the complete repair of vision. The advancements are carefully tracked to ensure positive developments.
- 04:Minimally Invasive and Promising Approach: Stem cell therapy provides a kind and convenient method for patients. Many therapies do not include major surgeries, making the patient more comfortable with shorter recovery times. Targeting the cells exactly where the treatment is required promotes greater success rates. This therapy would be highly beneficial to delicate patients, especially those with serious cases related to the retina. Doctors primarily focus on the safety, comfort, and observation of patients. Aftercare plays a crucial role in the success of the therapy. Researchers continue to work on optimizing the process and increasing success rates, keeping the therapy of retinal detachment on a positive tract.
GET STEM CELL TREATMENT FOR RETINAL DETACHMENT IN DELHI, INDIA
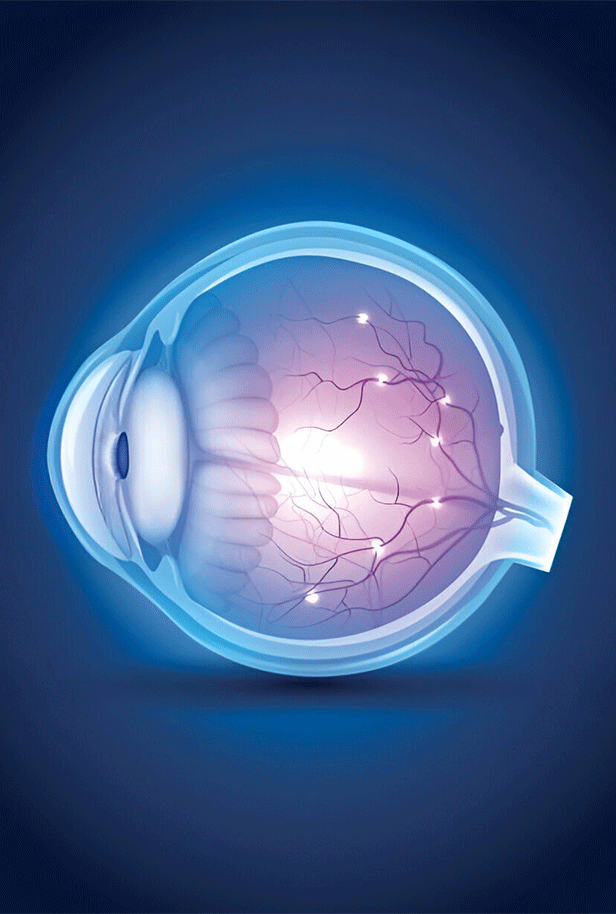
A thin layer of tissue (the retina) at the back of the eye detaches from its normal location, thereby creating a retinal detachment.
Separation of the retina’s cells from the nourishing layer of blood vessels that supplies oxygen and nutrients is known as retinal detachment. Your chance of irreversible vision loss increases when your retinal detachment goes unchecked.
Floaters and flashes appear unexpectedly, and your vision can suddenly be diminished. In order to better preserve the vision, the first step is to see an eye doctor (ophthalmologist).
Stem Cell Treatment for Retinal Detachment in Delhi, India
People are searching for stem cell therapy for Retinal Detachment in Delhi, India, but can’t seem to find the Best stem cell center or hospitals for Retinal Detachment at an affordable price. Global Stem Cell Care helps those patients to finding best hospitals for the Retinal Detachment stem cell treatment in Delhi, India
Do you know about Stem Cell Treatment for Retinal Detachment?
In the event that your retina has separated, you’ll definitely need surgery in order to fix it, hopefully within a brief time span of finding the problem. There are several considerations that decide the type of operation your surgeon prefers, such as how serious the detachment is. piercing the eye with a needle and pouring air or gas into it Pneumatic retinopexy is a surgical process in which a bubble of air or gas is inserted into the eye’s middle to help reshape the appearance of the cornea (the vitreous cavity).
Bubbles located in the right spot in the tear ducts are helpful in reducing the volume of fluid in the vitreous area behind the retina. During the operation, the doctor even uses cryopexy to close the retinal split.The fluid pools beneath the retina, and after the retina has adhered to the wall of the eye, the fluid will be drained. To keep the bubble in place, you can have to hold your head in an uncomfortable position for several days.
You should change the harness’s buckles to guarantee you can maintain your view unobstructed, and they’re normally fixed in place forever.Getting rid of the solvent and removing it.
The surgeon removes the vitreous, along with other tissue that is dragging on the retina, in this operation called vitrectomy (vih-TREK-tuh-me). When the vitreous has been removed, steam, silicone oil, or air is pumped into the eye’s interior to further flatten the retina.
Over time, the bubble will revert to its natural state on its own.
indenting the lining of the eye The surgeon stitches a slice of silicone to the white of the eye (sclera) over the affected region in this operation called scleral buckling. To alleviate some of the force exerted on the retina by the vitreous, this operation indents the wall of the eye.Your surgeon can also fashion a scleral buckle that surrounds your whole eye like a belt if you have many tears or gaps or an extensive detachment.
When the fluid has been drained, the vitreous area will refill with body fluid. If silicone oil was used, it could be surgically removed months afterwards, during the time span in which it could not be removed. Global Stem cell Care is offered by the Best stem cell center for Retinal Detachment. You can get help from the best and the most reliable experts.
In the event that your retina has separated, you’ll definitely need surgery in order to fix it, hopefully within a brief time span of finding the problem. There are several considerations that decide the type of operation your surgeon prefers, such as how serious the detachment is. piercing the eye with a needle and pouring air or gas into it Pneumatic retinopexy is a surgical process in which a bubble of air or gas is inserted into the eye’s middle to help reshape the appearance of the cornea (the vitreous cavity).
Bubbles located in the right spot in the tear ducts are helpful in reducing the volume of fluid in the vitreous area behind the retina. During the operation, the doctor even uses cryopexy to close the retinal split.The fluid pools beneath the retina, and after the retina has adhered to the wall of the eye, the fluid will be drained. To keep the bubble in place, you can have to hold your head in an uncomfortable position for several days.
Over time, the bubble will revert to its natural state on its own.
indenting the lining of the eye The surgeon stitches a slice of silicone to the white of the eye (sclera) over the affected region in this operation called scleral buckling. To alleviate some of the force exerted on the retina by the vitreous, this operation indents the wall of the eye.Your surgeon can also fashion a scleral buckle that surrounds your whole eye like a belt if you have many tears or gaps or an extensive detachment.
You should change the harness’s buckles to guarantee you can maintain your view unobstructed, and they’re normally fixed in place forever.Getting rid of the solvent and removing it.
The surgeon removes the vitreous, along with other tissue that is dragging on the retina, in this operation called vitrectomy (vih-TREK-tuh-me). When the vitreous has been removed, steam, silicone oil, or air is pumped into the eye’s interior to further flatten the retina.
When the fluid has been drained, the vitreous area will refill with body fluid. If silicone oil was used, it could be surgically removed months afterwards, during the time span in which it could not be removed. Global Stem cell Care is offered by the Best stem cell center for Retinal Detachment. You can get help from the best and the most reliable experts.
Symptoms of Retinal Detachment
Retinal removal is painless in itself. However, warning signals nearly often occur before anything arises or has escalated, such as:
The best stem cell treatment hospital for Retinal Detachment in Delhi extends the most reliable treatment for Retinal Detachment.
-
- The unexpected presence of several floaters,
- Small specks that continue to drift through the field of view (photopsia) Blurred vision
- A curtain-like shadow over the visual area steadily eliminates side (peripheral) vision.
Diagnosis of Retinal Detachment
To diagnose a retinal detachment, your doctor may employ the use of various tests, instruments, and procedures, including:
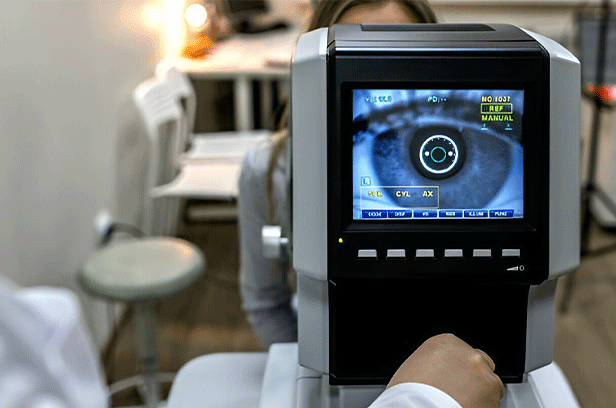
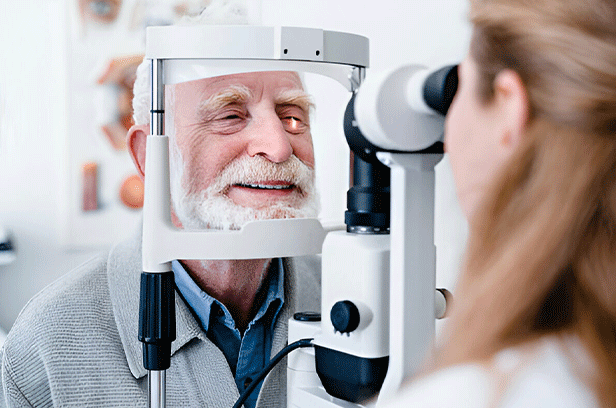
- Retinal examination. Using a special instrument with a bright light and lenses, the doctor can examine the back of your eye, including the retina. This type of device provides a highly detailed view of your whole eye, allowing the doctor to see any retinal holes, tears or detachments.
- Ultrasound imaging. If your eye has experienced bleeding, potentially making it hard to view your retina, your doctor may use this test.
Your doctor will likely examine both eyes even if you have symptoms in just one. Your doctor may ask you to return in a few weeks for a follow-up visit if a tear is not identified during the current appointment. This is to make sure that your eye has not developed a delayed tear due to the same vitreous separation. Also, if you experience new symptoms, it’s important to return to your doctor right away.
Types
Rhegmatogenous Retinal Detachment
- Central vision loss
- A straight line that suddenly appeared curved
- Brief flashes of light in the extreme peripheral part of the vision
- A sudden dramatic increase in the number of floaters
- The impression that a veil or curtain was drawn over the field of vision
- The appearance of rings and halos to the temporal side of the central vision
Tractional Retinal Detachment
- Gradual diminution of vision
- Central visual loss if the macula is detached
- Visual field defect, which usually progresses slowly
- A sudden drop in sight if associated with vitreous hemorrhage
Exudative Retinal Detachment
- Increase in the number of floaters
- Loss of peripheral vision
- Blurred vision
- A drape-like outline over your field of vision
The three causes of retinal detachment are:
- Rhegmatogenous: The most common cause of retinal detachment happens when there’s a small tear in your retina. Eye fluid called vitreous can travel through the tear and collect behind the retina. It then pushes the retina away, detaching it from the back of your eye. This type of detachment usually happens as you get older. As the vitreous shrinks and thins with age, it pulls on the retina, tearing it.
- Tractional: Scar tissue on the retina can pull it away from the back of the eye. Diabetes is a common cause of these retinal detachments. The prolonged high blood sugar can damage blood vessels in your eye, which can result in scar tissue formation. The scars and areas of traction can get bigger, pulling and detaching the retina from the back of the eye.
- Exudative: Fluid builds up behind the retina despite no retinal tear. As the fluid collects, it pushes your retina away. The leading causes of fluid buildup are leaking blood vessels or swelling behind the eye, which can happen from such causes as uveitis.
Gene Therapy
Gene therapy involves the modification of defective deoxyribonucleic acid (DNA) in recipient cells or tissues to achieve a desired therapeutic effect. Retinal dystrophies are usually symmetrical and bilateral, allowing one eye to serve as a control in clinical trials. Gene therapy involves a cloned copy of the wild-type gene linked to a particular condition, a promoter that controls the gene expression specifically in the target cells, and a vector/carrier, which is usually a virus stripped of its replicative and virulent features, which can act as a cargo and deliver the necessary gene into the target cells of the host.
Nutrition Therapy
Medical nutrition therapy (MNT) is a treatment technique developed and supervised by a physician to treat medical disorders and their resulting effects through a specially adapted diet. The treatment seeks to correct dietary inefficiencies and metabolic imbalances to provide the stem cells with the best available environment to mature correctly and improve the overall health of the patient. One may observe floaters, black spots, reduced central vision, diffuse haziness, drop in low contrast vision, wavy vision or flashes of light. These floaters might settle and appear sporadically. However, flashes of light occur occasionally for a few days to weeks. One must consult a retina specialist in case of these symptoms.
SANAYA SINGH FROM TEXAS VISITED INDIA FOR STEM CELL THERAPY
I was diagnosed with retinal detachment, and my doctor told me that I needed an operation to repair the detached retina. I didn’t want surgery, so I started looking for alternative treatments. When I found stem cell therapy, I was very excited and a little nervous at the same time. It sounded less painful and was less expensive than surgery. I went for it. I got it, and I’m happy to report that my vision is way better after just a few months, and I can see things. And I want to thank the whole team of Global Stem Cell Care.
MARK SMITH FROM NEW YORK CAME TO US FOR THE TREATMENT OF RETINAL DETACHMENT VIA STEM CELLS
Hi, I am Mark from New York, and I visited India with my wife for the treatment of retinal detachment. I had a retinal detachment and was terrified to go through surgery and recovery time. Due to this fear, I searched for an alternative treatment to cure my condition, and then I found that stem cell treatments were very effective and less time-consuming, and I am thrilled with the results. I will suggest it to anyone who has the same problem.
AIMAN FROM DUBAI VISITED INDIA FOR STEM CELL THERAPY TO TREAT RETINAL DETACHMENT
I was detected with retinal detachment, and then my friend suggested this stem cell treatment, and to be honest, it helped me a lot. So, if you are looking for something affordable and effective, I highly recommend this treatment, and the best part is that it has no side effects to worry about. We reached India in a few days because of the support they are offering. They helped to get a visa to visit India because of my condition, and their staff picked me up from the airport, and the doctors were well educated.
JOSH MATHEW’S SUCCESS STORY OF RETINAL DETACHMENT THROUGH STEM CELL TREATMENT
My doctor recommended a stem cell treatment. I couldn’t get the treatment done in my country, so I got on a plane and went to Global Stem Cell Care in India. The stem cell treatment is available to anyone. The cost was much less than it would have cost me in my own country, and the results were amazing. I had my treatment done a few months ago, and I haven’t had any eye problems since then. I can see well than I did before my retinal detachment.
Related Disorders for Stem Cell Treatment
optic nerve damage stem cell treatment
stem cell therapy age related macular degeneration
stem cells cure retinitis pigmentosa
is there a cure for optic nerve hypoplasia
optic neuropathy stem cell treatment
eye best’s disease treatment with stem cells
Implantation
The following is the structure that is followed during the implantation stage:
MECHANISM
A clinical trial using stem cell transplantation has potential as a possible cure for some vision-destroying retinal degenerative diseases, including retinitis pigmentosa, that currently leave patients blind. Results from a number of Phase I/II clinical trials in the field of stem cell treatment for Retinal Detachment in India have recently been available for the first time. This clinical trials, which are normally managed in conjunction with universities, are focused on well-established animal science and are set on ensuring patient welfare. However, in other poorly controlled treatment institutions, accounts of significant adverse effects have surfaced in the lay and science press. As with other advances in stem cell treatment for blindness, success in this field has met with an outpouring of interest from patients, academics, physicians, and the medical and pharmaceutical industries. The positive news, though, is that there have been notable issues posed about the efficacy of stem cell therapy for Retinal Detachment in Delhi, which may raise questions about patient health. The aim of this study is to outline and assess the safety of human retinal stem cell transplantation as a possible therapy for retinal degenerative diseases.

MECHANISM
A clinical trial using stem cell transplantation has potential as a possible cure for some vision-destroying retinal degenerative diseases, including retinitis pigmentosa, that currently leave patients blind. Results from a number of Phase I/II clinical trials in the field of retinal stem cell transplantation have recently been available for the first time. This clinical trials, which are normally managed in conjunction with universities, are focused on well-established animal science and are set on ensuring patient welfare. However, in other poorly controlled treatment institutions, accounts of significant adverse effects have surfaced in the lay and science press. As with other advances in stem cell treatment for blindness, success in this field has met with an outpouring of interest from patients, academics, physicians, and the medical and pharmaceutical industries. The positive news, though, is that there have been notable issues posed about the efficacy of retinal stem cell transplantation, which may raise questions about patient health. The aim of this study is to outline and assess the safety of human retinal stem cell transplantation as a possible therapy for retinal degenerative diseases.
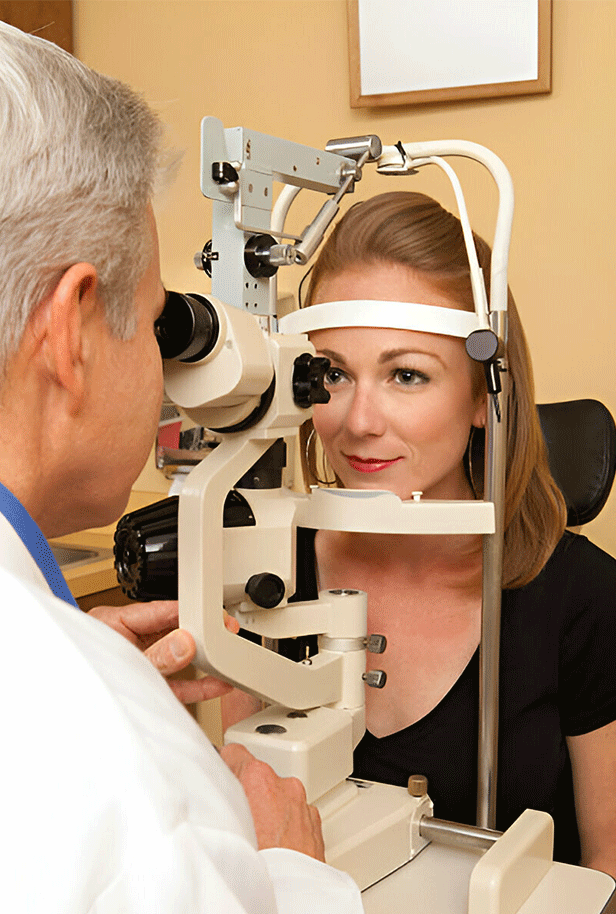
Get Stem Cell Therapy for Retinal Detachment in Delhi
Stem cell therapy has many benefits for the care of the skin. In terms of costs, a low amount of stem cells is needed. With current imaging techniques, the process of transplantation is very straightforward, and transplanted cells can be tracked easily. To be able to change the fellow eye, it can be used. Furthermore, as the immune privilege of the eye remains, long-term immunosuppressive therapy is not necessary.
Scientists conducting clinical trials have found that implantation of healthy stem cells instead of degenerated retinal cells has enabled the production of new intercellular connections, cell regeneration, and changes in vision. While stem cells have the ability to differentiate into multiple cells in their environment, including retinal neural cells and photoreceptors, they are particularly adept at differentiating into cells that are already present. Although previous laboratory research has shown that a retinal detachment stem cell treatment in Delhi is very consistent with retinas and are able to respond to bipolar, amacrine, horizontal, and glial cells, as well as photo receptors. This current study demonstrates that stem cells are much better at taking on Müller, amacrine, bipolar, horizontal, and glial cells as well as photo receptors.
Bone marrow- and adipose tissue-derived ESCs, IPSCs, and MSCs are used in stem cell treatment for retinal diseases in India. Stem cell therapy for Retinal Detachment by the best stem cell hospital ensures that you have the best treatment that you need to fight the Retinal Detachment trouble.
HOW GLOBAL STEM CELL CARE THERAPY WORKS?
ESCs Discharge – Clusters of egg cells, removed in the first three to five days of embryonic development, are grown in a laboratory to construct the ESCs. This type of pluripotent cell is known as stem cells since they can divide into all cell types that are produced from the ectoderm, mesoderm, and endoderm. We will remove these cells and the embryo will be unharmed.
Mesenchymal stem cells (MSCs) are adult stem cells. Tumor tissue cultures produce significant concentrations of these lipids, which are usually present in the tissues from which they are derived, including blood, blood vessels, skeletal muscles, skin, teeth, bone marrow, fat, and cartilage.
Most widely used MSCs are produced from either fat or bone marrow. Multipotent cells
are assigned this classification because they are capable of differentiating into various cell types in the body.
The IPSCs are created when cells originating from adults are transformed in vitro using in vitro genetic reprogramming, which gives them ESC properties. They are like ESCs in that they have the potential to shape many forms of tissue, also known as multipotency
Three types of cord blood stem cells
- These were separated in a lab dish from the blood cells collected during delivery.
- The amniotic fluid stem cells can be derived from an amniotic fluid extract from the birth mother.
- Amniotic fluid amnion collected in vitro provides a supply of differentiated amniotic epithelial cells.
ESCs Discharge – Clusters of egg cells, removed in the first three to five days of embryonic development, are grown in a laboratory to construct the ESCs. This type of pluripotent cell is known as stem cells since they can divide into all cell types that are produced from the ectoderm, mesoderm, and endoderm. We will remove these cells and the embryo will be unharmed.
Mesenchymal stem cells (MSCs) are adult stem cells. Tumor tissue cultures produce significant concentrations of these lipids, which are usually present in the tissues from which they are derived, including blood, blood vessels, skeletal muscles, skin, teeth, bone marrow, fat, and cartilage.
Most widely used MSCs are produced from either fat or bone marrow. Multipotent cells are assigned this classification because they are capable of differentiating into various cell types in the body.
The IPSCs are created when cells originating from adults are transformed in vitro using in vitro genetic reprogramming, which gives them ESC properties. They are like ESCs in that they have the potential to shape many forms of tissue, also known as multipotency
Three types of cord blood stem cells
- These were separated in a lab dish from the blood cells collected during delivery.
- The amniotic fluid stem cells can be derived from an amniotic fluid extract from the birth mother.
- Amniotic fluid amnion collected in vitro provides a supply of differentiated amniotic epithelial cells.
VIP TREATMENT TO PATIENTS AT GLOBAL STEM CELL CARE
- The stem cell therapy for Retinal Detachment services given to patients at Global Stem Cell Care takes place in the VIP recovery room of the advanced hospital.
- The 24/7 on-site nursing team maintains round-the-clock supervision of the patients.
- Global Stem Cell Care recommends that patients stay in the hospital for at least three days following their surgery.
GLOBAL STEM CELL CARE TREATMENT PROCEDURE
The treatments that take place in Global Stem Cell Care are of 3 days. The treatment protocol is safe and non-invasive. The patients can travel the next day. The following is the day-wise schedule for the patients.
Pick up from the Airport to theHospital
Interaction between Dr and Patient, to clear all their doubts at that time
Admission procedure
Clinical examination & Lab test will be done prescribed by the doctor
Supportive Therapy
Stem cell Procedure
Supportive therapies
Physiotherapy
Supportive Therapy
Physiotherapy
Discharging formalities
Drop back to the Airport
- For Admission, carry the identity card (Passport/ Pan Card / Driving License)
- Carry the hard copy of Patient reports
Our Promise
Global Stem Cell Care promises you to provide the best retinal detachment stem cell therapy for our patients. We are committed to harness the regenerative potential of stem cells to restore vision and enhance quality of life. Our doctor uses the latest technologies and techniques to make the treatment better for you, so that you don’t get any problems during the procedure. You can get a friendly environment in our best stem cell center for retinal detachment. We don’t just provide hope, we offer new life to those who are suffering from retinal detachment.


Cost
Retinal detachment refers to that condition when a thin layer of tissue detached from its area. To treat this condition in an effective way, stem cell therapy offers hope to the people who are suffering from retinal detachment. But stem cell treatment for retinal detachment in India can be expensive because it has the capabilities to differentiate into specialised cell types. There are some other factors that make this treatment option expensive such as the condition of your disease, type of stem cell you want to use, the type of your condition, and many other factors. You can see additional factors that may fluctuate the cost including diagnosis, consultancy fees, transportation, etc. With the help of our researchers, we are trying to make this treatment affordable to ensure everyone will live their quality life.
Success Rate
At Global Stem Cell Care, we feel proud to treat your retinal detachment with the help of stem cell therapy. These cells have the regeneration ability to restore damaged retina tissue which helps to reduce the symptoms. The success rate of stem cell therapy for Retinal Detachment in Delhi depends on many factors such as age of the patient, stem cell they choose, medical history, etc. Stem cells offer hope to various individuals and you can see it in our testimonial section. But the success rate does not go the same for every patient. There are many patients who experience remarkable results while others get temporary relief. Stem cell therapy is still under process and our researchers are doing hard work to make it successful for all.


Advantages
Stem cell treatment can be an effective and innovative approach to treat retinal detachment. There are several reasons that shows why people are considering this treatment option and some of them are:
- Regeneration: Stem cells have the remarkable ability to differentiate into various cell types, including retinal cells. This enables them to regenerate damaged retinal tissue, potentially restoring vision.
- Precision: Stem cell therapy allows for precise targeting of damaged areas within the retina, promoting localised repair and minimising collateral damage.
- Reduced Risk of Rejection: Stem cells can be derived from the patient’s own body (autologous transplantation), reducing the risk of rejection and eliminating the need for immunosuppressive drugs.
- Minimised Side Effects: Compared to traditional treatments like surgery or laser therapy, stem cell therapy typically involves minimally invasive procedures, reducing the risk of complications and side effects.
- Long-term Benefits: Stem cell treatments have the potential to provide long-lasting improvements in vision, addressing the underlying cause of retinal detachment rather than just managing symptoms.
- Personalised Medicine: Stem cell therapy can be tailored to each patient’s unique needs, offering personalised treatment plans for optimal outcomes.
Quality Control
Quality control for retinal detachment treatment via stem cell therapy at Global Stem Cell Care ensures efficacy and safety through meticulous protocols:
- Patient Screening: Rigorous evaluation of patient suitability based on medical history and diagnostic tests.
- Stem Cell Sourcing: Ethical procurement of stem cells adhering to international standards.
- Procedure Standardisation: Adherence to standardised procedures for consistency and reproducibility.
- Sterility Assurance: Strict measures to maintain sterile conditions during cell processing and administration.
- Monitoring Protocols: Regular monitoring post-treatment to track progress and detect any adverse reactions.
- Continuous Improvement: Feedback-driven system for continual refinement of protocols to enhance outcomes.
Quality Certificate
Global Stem Cell Care proudly announces its Quality Certificate for treating retinal eye detachment with stem cell therapy. Employing cutting-edge techniques and expert medical professionals, our center ensures top-tier care and unparalleled results. Our commitment to excellence is evident in our rigorous quality standards, patient-centric approach, and adherence to international medical guidelines. Through meticulous evaluation, personalised treatment plans, and continuous follow-up, we strive to achieve optimal outcomes for every patient. With this Quality Certificate, patients can trust in our dedication to providing safe, effective, and innovative stem cell therapy for retinal eye detachment, offering hope and vision for a brighter future.

What to Expect from Stem Cell Treatment for Cerebral Palsy?
By definition, pluripotent stem cells (PSCs) can differentiate into both endodermal, mesodermal and ectodermal lineages. First cultivated in 1998, human embryonic stem cells (hESCs) have the ability to differentiate into all types of cells. They are a promising target for stem cell-based treatment, but they pose possible ethical concerns, including foetal progenitor cells.
Induced pluripotent stem cells (iPSCs) are a subtype of pluripotent stem cells that derive from a differentiated source of cells, such as skin fibroblasts or blood cells; certain immunological problems associated with hESC-based therapies can be deemed less controversial and may be negated. Since they are not pluripotent, but do create some of the cell types of their host tissue,
somatic stem cells, such as bone marrow, adipose, central nervous system and umbilical stem cells, are distinct from ESC or iPSC-based therapies.
Since they are not pluripotent, but do create some of the cell types of their host tissue, somatic stem cells, such as bone marrow, adipose, central nervous system and umbilical stem cells, are distinct from ESC or iPSC-based therapies.
Given the unmet therapeutic need, the comparatively immune-privileged location and the transparent ocular media that facilitates direct visualisation of transplanted cells, it turns out that the eye is a strong choice for stem cell clinical study.
![]() ong-term trials have shown that 5 percent-14 percent of patients may experience new breaks in the retina even after preventive treatment of a retinal hole or tear, which could lead to retinal detachment.
ong-term trials have shown that 5 percent-14 percent of patients may experience new breaks in the retina even after preventive treatment of a retinal hole or tear, which could lead to retinal detachment.
![]() Overall, however, with the return of usable vision to many thousands of persons, rehabilitation of retinal detachments has taken great strides in the past 20 years.
Overall, however, with the return of usable vision to many thousands of persons, rehabilitation of retinal detachments has taken great strides in the past 20 years.
![]() A dilated examination of the non-operated eye will also be conducted due to an elevated risk of retinal detachment of the other eye. L
A dilated examination of the non-operated eye will also be conducted due to an elevated risk of retinal detachment of the other eye. L
![]() Therefore, close follow-up by an ophthalmologist is required and visits will include a slit lamp examination and a dilated retinal and vitreous examination.
Therefore, close follow-up by an ophthalmologist is required and visits will include a slit lamp examination and a dilated retinal and vitreous examination.
![]() High resulting occurrence of cataracts is consistent with pars plana vitrectomy and the use of intraocular gas in the phakic eyes (eyes containing the natural lens).
High resulting occurrence of cataracts is consistent with pars plana vitrectomy and the use of intraocular gas in the phakic eyes (eyes containing the natural lens).
![]() Where a gas or air bubble has been injected into the eye during surgery, it is often necessary to preserve the correct orientation of the head to assess the final outcome.
Where a gas or air bubble has been injected into the eye during surgery, it is often necessary to preserve the correct orientation of the head to assess the final outcome.
![]() It can develop new cracks, tears, or dragging, leading to new detachments of the retinal. Scarring due to subretinal fibrosis can be present (development of scar tissue beneath the retina).
It can develop new cracks, tears, or dragging, leading to new detachments of the retinal. Scarring due to subretinal fibrosis can be present (development of scar tissue beneath the retina).
Possible Improvement
In about 85 percent of patients with a single vitrectomy or scleral buckle operation, the surgical reconstruction of retinal detachment is successful. About 95% of retinas are successfully re-attached with further surgery. However, several months can pass before the vision comes back to its final stage. Several variables depend on the ultimate outcome of the view. For example, because of degenerative changes in the macula, central vision rarely returns to normal after the macula is removed. The vision changes in this case are close to those found in macular degeneration, a much more common disorder (age-related macular degeneration or ARMD). And if the macula has not been detached, there might also be any vision missing, but much would be restored.
FOLLOW UP
The follow up is the most important stage through which the doctors make the assessment of the condition of the patient. Without the follow-up, the treatment of Cerebral Palsy cannot be completed. According to the doctor’s recommendation, the patient has to come to visit.
FREQUENTLY ASKED QUESTIONS
Q. What are the retinal detachment risk factors?
A. Factors that may increase the risk of retinal detachment include:
Inherited retina anomalies frequently associated with myopia (near-sight) • ageing
Face trauma Eye surgery Glaucoma Different retinal and macular disorders Diabetes Diabetes Diabetes Family history of retinal issues
Q. Is retinal detachment linked to a surgeon's error during eye surgery?
A. Oh, no. Following uncomplicated eye surgery carried out at the highest degree of excellence, retinal cracks, splits, or tears may occur.
Q. What kind of damage will lead to detachment of the retina?
A. Direct eye damage may result in retinal cracks, gaps, or tears occurring days, weeks, months, or even years after the occurrence.
How do stem cells repair retinal tissue?
Stem cells help replace damaged retinal cells and tissues. They promote natural regeneration of photoreceptors and integrate into retinal layers effectively. Growth factors released by the cells improve nerve signal transmission to the brain. Early intervention enhances therapy effectiveness, while continuous monitoring ensures proper healing. The approach focuses on both structural and functional repair. Patients may notice gradual vision improvement, although results vary depending on injury severity.
Can stem cells restore peripheral vision?
Peripheral vision can often be compromised after the retinal separation. Stem cell treatment has great potential in maintaining retinal nerve functions and can even improve the peripheral vision. The treatment at the right time increases the possibilities of full recovery and maintaining the whole vision field. Most patients have reported progressive improvements in the orientation and mobility dexterities. The treatment response depends upon the extent of retinal separation and requires regular follow-ups to assess the response. The peripheral vision improvements can be increased with the aid of other supportive modalities.
How is therapy personalized for each patient?
Doctors carefully assess retinal damage before planning treatment. Variables such as the patient’s age, health, and the level of retinal detachment are taken into consideration before any form of therapy is chosen. The amount of stem cells needed and the method of administration are carefully selected to achieve the highest possible benefit. The follow-up regimens are individualized according to the patients’ needs for healing.
Can stem cells prevent recurrent detachment?
Stem cells aid in strengthening the retinal tissue, reducing inflammation, as well as protecting the healthy cells that remain, which could aid in preventing retinal detachment in the future. Starting the treatment early helps in promoting stability in the tissues as well as proper vision. Close monitoring of the retinal health by professionals, including follow-up care, is vitally important. Although stem cells do not provide a complete substitute for surgery, treatment along with surgery could prove fruitful.
How do doctors ensure stem cell survival in the retina?
Doctors use advanced imaging to locate damaged retinal areas precisely. Stem cells are prepared under strict laboratory conditions for maximum viability. Protective solutions support cell survival during delivery. Targeted placement ensures cells reach injured retinal tissue effectively. Doctors monitor integration and regeneration over time. Post-treatment care prevents infection or inflammation. Follow-ups confirm cells are functioning properly. Personalized protocols optimize survival for each patient. Early intervention further increases effectiveness. Continuous observation ensures long-term therapy success.
How soon can visual improvements appear?
The effects of stem cell therapy are progressive and can take weeks or months for improvement. Initial improvements can be seen in light perception, and later on, improvements in contrast sensitivity and visual clarity can be achieved. The level of retinal damage and the patient’s age factor greatly in the recovery of the eye. Regular follow-ups can greatly increase the chances of successful outcomes, and even slight improvements are beneficial for patients undergoing stem cell therapy.
Are multiple therapy sessions required?
Some patients require more than one session to maximize results. Additional doses can boost retinal regeneration and improve functional recovery. Doctors evaluate retinal response before scheduling repeat treatments. The timing of sessions depends on healing speed and patient age. Not every patient needs multiple therapies. Carefully planned follow-ups ensure safety and effectiveness. Personalized treatment plans help achieve the best long-term outcomes and support retinal health.
Can stem cells improve night vision?
Night vision often suffers after retinal detachment. Stem cells support photoreceptor repair and improve retinal signaling, which may enhance low-light vision. Patients may notice gradual improvement in dim lighting conditions. Early treatment increases the likelihood of night vision recovery. Therapy effects vary depending on severity, and complementary visual training may further support improvement. Gradual functional gains enhance daily activities and overall quality of life.
How is therapy success measured?
Success is evaluated through functional vision tests and retinal imaging. Doctors assess light perception, visual field, contrast sensitivity, and tissue repair. Patient-reported vision improvements are also considered. Even small functional gains are significant and indicate that a therapy is working. Follow-up thereafter detects changes occurring over time and refines the approach in an appropriate manner. Long-term follow-up seeks durable results and augments the maintenance of visual improvements afforded by treatment.
Is stem cell therapy safe for Indian patients?
Generally, stem cell therapy is safe if executed by qualified doctors in the particular field. All procedures follow very strict clinical and ethical standards. The risk involved in this type of treatment is less than in traditional surgery because most of the patients experience mild discomfort or irritation. Infection risk remains low thanks to sterile techniques. Physicians with experience can deliver precisely with appropriate post-treatment care. Sensitive patients, including children, can also undergo the treatment, and continuous monitoring helps to safely recover.
Can therapy help chronic retinal detachment?
Chronic retinal detachment cases are challenging but can benefit from stem cell therapy. Stem cells support residual retinal tissue and promote gradual repair. Functional stabilization may occur, slowing further vision loss. Early evaluation increases benefits, and combined supportive treatments may enhance results. Recovery is gradual, and outcomes vary individually. Doctors provide realistic expectations and maintain continuous monitoring to ensure the best possible visual improvement.
What is the future of retinal stem cell therapy in India?
Stem cell therapy for retinal detachment is rapidly advancing in India. Specialized centers continually improve techniques and treatment protocols. Clinical studies optimize safety and therapy effectiveness. Personalized approaches are emerging, offering better patient outcomes. Accessibility to advanced therapy is increasing across major cities. Ongoing research focuses on higher cell survival rates and long-term functionality. Innovation provides hope for patients, making the future of retinal care promising.
Conclusion:
Stem cell therapy is creating a silent revolution in the treatment of retinal detachment in India. The therapy is based on repairing defective retinal cells and positioning vision to heal step by step. The cells support the body’s inherent healing mechanism and also function very well in lining up in retinal tissues. Early intervention in treatment usually proves to be more beneficial in this therapy, while regular follow-ups are also important to ensure healthy healing as well as changes if required.
In addition to repairing harmed cells, this treatment also serves to preserve unaffected cells in the retina while reducing inflammation and slowing progression. The stabilization achieved also maintains vision and fosters independence in performing daily tasks. Minute improvements also make great impacts in terms of increasing the quality of life. Treatments will be customized depending on individual conditions and needs, and follow-through is vital in monitoring progress.
The method is MII and can be considered highly tolerable compared to major surgery. The cell survival and potency can be improved with targeted delivery, and pain and safety are taken into account. Furthermore, it could be considered with vision therapy or any approach that provides better success.
The advancements made in India in regenerative eye care are quite impressive, thanks to the centres that are promoting innovative solutions. Even today, research revolves around safety, efficiency, and custom treatment plans but with continuous innovations, stem cell therapy remains a shining hope for patients with retinal detachment.
Treatment Disclaimer:
We provide consultation, case evaluation, and patient support services in the field of regenerative medicine. As per current medical guidelines in India, stem cell-based interventions (other than approved indications) are considered investigational and are available only within regulated clinical research settings. For patients exploring broader options, we also assist in facilitating access to treatment pathways, including internationally accredited centers where different regulatory frameworks may apply.
Useful Tags
Stem Cell Treatment for Retinal Detachment, Stem Cell Therapy for Retinal Detachment in India, Stem Cell Therapy for Retinal Detachment Cost in India, Affordable Stem Cell Therapy for Retinal Detachment in India, Low Cost Stem Cell Therapy for Retinal Detachment in India, Price of Stem Cell Therapy for Retinal Detachment in India, stem cell treatment for Retinal Detachment in Delhi, stem cell treatment for Retinal Detachment in India, stem cell Hospital for Retinal Detachment in Delhi, stem cell Hospital for Retinal Detachment in India